United Health Group is the largest health insurance company in the United Stated of America, Ingenix is their software division. Ingenix is the largest software company for classifying and managing medical procedures.
I was contracted to design new features and optimize existing functionality for the Transact 360 – Provider, claims management and arbitration software suite, bringing this product from Alpha to General Availability release. Transact 360 software is the leading enterprise software suite for Provider Organization revenue recovery and appeals process, within the Health Care industry.
Methodology: Scrum, 6 week iterations
Skills Used:
- Business objectives analysis, Roadmap development.
- Interviewed Customers for requirements gathering.
- Requirements analysis and development.
- Validated Requirements twice weekly with Customers.
- Task and Work Flow analysis and development.
- Validated Flows with Customers regularly.
- Wire Frames, Annotated Prototypes, click through HTML Prototypes.
- Validated Prototypes with Customers regularly.
- Design common user interface standards, usability and design guidelines.
Example Assignment: Design new TransContract 360 features for Provider Organizations to manage contracts with Insurers and arbitrate claims, which were incorrectly processed.
Design Opportunity: TransContract 360 Provider was designed for visibility into complex contractual issues and batch submittal of incorrect claims for appeal. Up to 30 % of all health insurance claims are processed incorrectly, which is a major problem for the health care industry in the United States of America.
My job was to design new features for the TransContract 360 application in order to bring it from the Beta release to the General Availability Release.
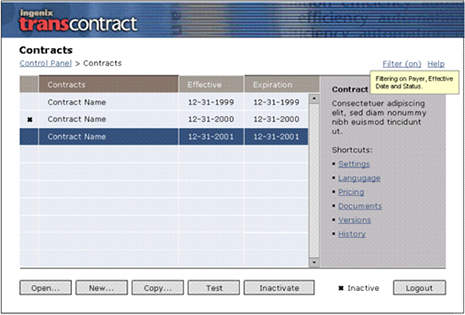
TransContract Provider Control Panel: The new interface was designed to allow for simple access to contracts with the ability to deep dive into detailed settings.
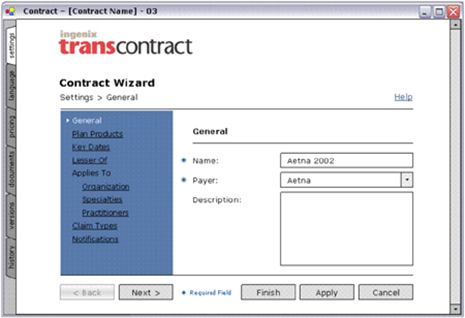
Create New Contract Module: Abstracting contracts and creating rules, which would be used to validate millions of diverse claims, based on any number of procedures.